Sciatica is one of the most common and frustrating nerve-related conditions, often causing persistent pain that radiates from the lower back down the leg. As regenerative medicine continues to evolve, many practitioners are asking a key question: Does PRP work for sciatica?
Platelet-rich plasma (PRP) therapy has gained attention as a minimally invasive option that may support tissue healing and reduce inflammation. But outcomes can vary—and for clinics, results are not only about technique, but also about the quality of PRP preparation tools, especially the tubes used during processing.
In this guide, we’ll first explain how PRP therapy interacts with sciatic conditions, then consider what clinical evidence suggests, and finally explore how to select the right PRP systems for consistent outcomes.
Does PRP Work for Sciatica? Understanding the Mechanism
To understand whether PRP helps sciatica, we first need to look at the cause. Sciatica is typically linked to nerve irritation or compression, often due to:
- Herniated discs
- Degenerative disc disease
- Spinal stenosis
- Muscle inflammation affecting the sciatic nerve
PRP works differently from traditional treatments. Instead of masking pain, it aims to stimulate healing at the source.
PRP is derived from the patient’s own blood and contains a high concentration of platelets, which release growth factors such as:
- PDGF (Platelet-Derived Growth Factor)
- TGF-β (Transforming Growth Factor Beta)
- VEGF (Vascular Endothelial Growth Factor)
These factors may help:
- Reduce inflammation around the nerve root.
- Promote soft tissue repair.
- Improve local blood supply.
So, does PRP work for sciatica?
The answer is that it can, particularly in cases where inflammation—not severe structural compression—is the primary driver.
Clinical Evidence: Does PRP Work for Sciatica in Practice?
Most top-ranking medical articles agree on one thing: PRP is not a universal cure, but it shows promising results in selected patients.
Emerging clinical observations suggest:
- PRP injections near affected nerve roots may reduce pain intensity
- Some patients report longer-lasting relief compared to steroid injections.
- PRP avoids the degenerative side effects associated with repeated corticosteroids
However, results depend heavily on:
- Injection accuracy (often guided by ultrasound or fluoroscopy)
- Patient condition (acute vs chronic sciatica)
- PRP quality and concentration
This last point is often overlooked. Inconsistent platelet concentration—often caused by low-quality PRP tubes or poor separation performance—can directly affect outcomes.
That’s why many clinics are shifting toward standardized systems such as:
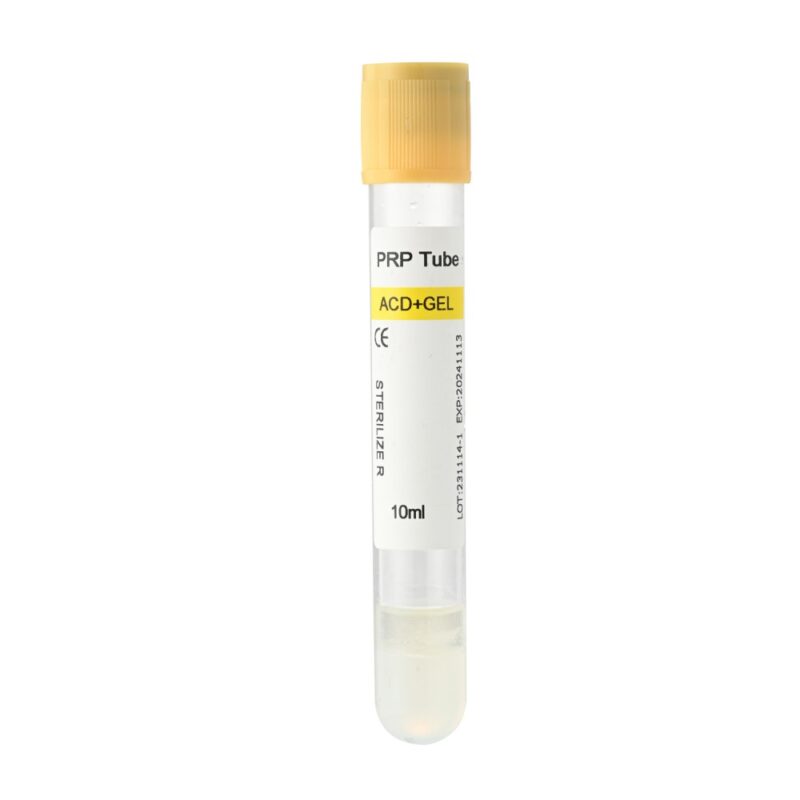
- ACD + Gel PRP Tube (Yellow Top)
- 10ml ACD+Gel+Biotin PRP Tube for Hair & Tissue Repair
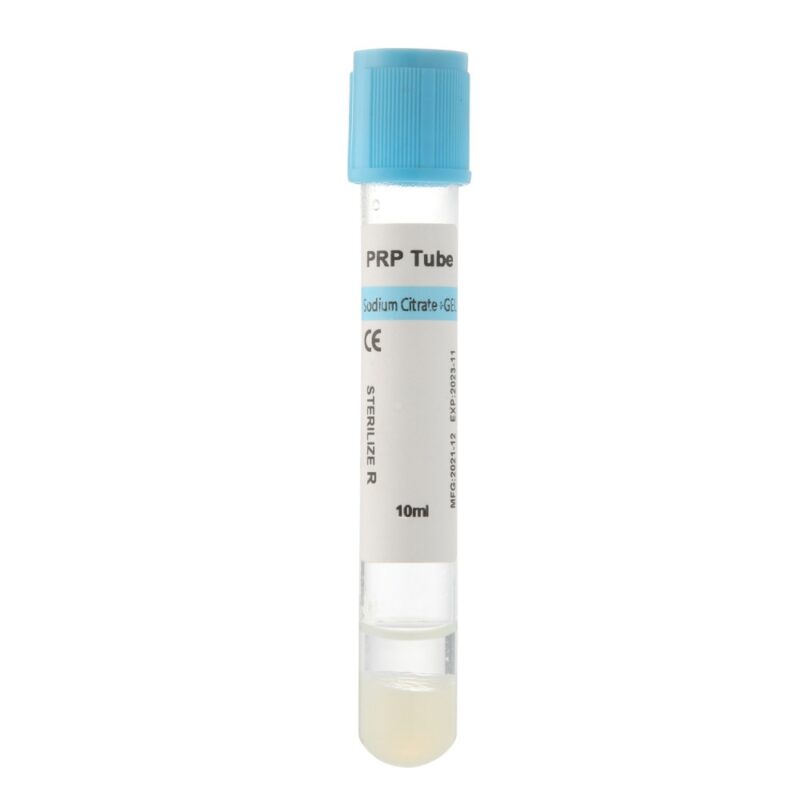
- Sodium Citrate Gel PRP Tube for Orthopedic Applications
If you’re evaluating whether PRP works for sciatica in your clinic, it’s worth reviewing not just the technique, but also your PRP preparation protocol and consumables. For reference-grade tubes and specifications, you can explore options through Siny PRP.
How PRP Therapy Is Performed for Sciatica
A typical PRP procedure for sciatica follows a structured workflow:
1. Blood Collection
Blood is drawn into specialized PRP tubes containing anticoagulants such as ACD or sodium citrate.
2. Centrifugation
The sample is spun at controlled speeds to separate layers:
- Red blood cells (bottom)
- Platelet-rich plasma (middle/top)
3. PRP Extraction
The concentrated platelet layer is carefully extracted.
4. Targeted Injection
PRP is injected near the affected nerve root or surrounding tissues under imaging guidance.
The quality of separation in Step 2 is critical. Poor gel stability or inconsistent tube materials can lead to:
- Low platelet yield
- Contamination with RBCs
- Reduced clinical effectiveness
That’s why clinics using systems like Siny PRP Tubes with medical-grade gel separators often report more consistent preparation results. If you’re refining your workflow, reviewing your consumables via Siny PRP is a practical next step.

Benefits and Limitations: Is PRP a Reliable Solution for Sciatica?
Potential Benefits
- Minimally invasive, outpatient procedure
- Uses autologous (patient-derived) material
- Lower risk of allergic reactions
- May provide longer-term relief than steroids
Limitations
- Not effective for severe nerve compression requiring surgery.
- Results vary depending on practitioner skill and equipment.
- Requires high-quality PRP preparation to be effective.
So again, does PRP work for sciatica?
It works best as part of a carefully controlled clinical protocol, not as a standalone quick fix.
Why Choosing the Right PRP Tube Supplier Matters
In many top-ranking articles, equipment quality is barely discussed—but in real clinical settings, it makes a significant difference.
A reliable PRP tube supplier ensures:
- Consistent anticoagulant ratios
- Stable gel separation performance
- High platelet recovery rates
- Sterility and compliance (ISO standards)
For distributors and clinics, this directly impacts:
- Treatment reproducibility
- Patient outcomes
- Brand reputation
When sourcing PRP tubes, it’s important to look beyond price and evaluate:
- Tube material (PET vs glass)
- Additive formulation (ACD-A, sodium citrate, gel quality)
- Manufacturing standards
If you’re comparing suppliers, reviewing product lines such as ACD+Gel PRP Tube, PRP Tube with HA, or Biotin-enhanced PRP systems through Siny PRP can help you benchmark specifications.
FAQ: PRP for Sciatica
1. Does PRP work for sciatica pain relief?
Yes, PRP may reduce inflammation and promote healing in certain types of sciatica, especially when caused by soft tissue irritation rather than severe compression.
2. How long does it take to see results?
Most patients begin to notice improvement within 2–6 weeks, with continued progress over several months.
3. Is PRP better than steroid injections?
PRP may provide longer-lasting results without the tissue damage risks associated with repeated steroid use, but outcomes vary.
4. How many sessions are needed?
Typically 1–3 sessions, depending on severity and patient response.
5. Does PRP quality affect treatment results?
Absolutely. Poor platelet concentration or contamination can significantly reduce effectiveness, making high-quality PRP tubes essential.
Summary
So, does PRP work for sciatica? The evidence suggests it can be an effective option for the right patients—particularly when inflammation plays a central role.
But successful outcomes depend on more than just the injection itself. From blood collection to centrifugation, every step matters—and that starts with choosing the right PRP preparation system.
For clinics and distributors looking to improve consistency and treatment performance, exploring well-designed PRP tube solutions through Siny PRP can be a practical step toward better results.